Index for
slide deck
Introduction
-1024x576.jpg)
Comorbidity
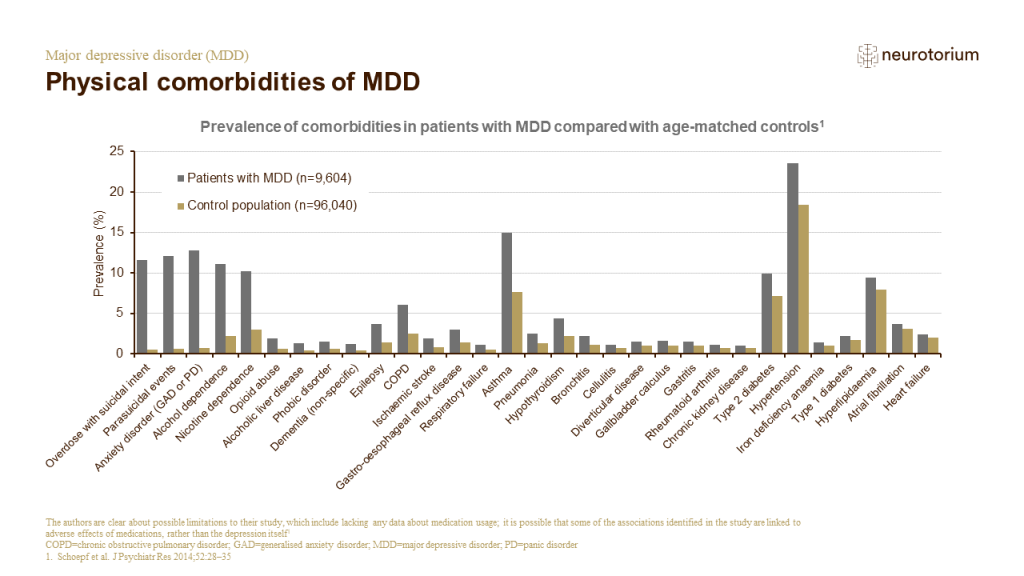
A retrospective analysis of patient data was performed to compare the prevalence of chronic conditions in patients with MDD. Of the total population studied, roughly one in ten had depression.
-1024x576.jpg)
Prevalence of chronic conditions in patients with MDD
In this study, data from the 2007 and 2009 releases of the Medical Expenditure Panel Survey (MEPS) were used.[Bhattacharya et al., 2014] The MEPS is a nationally representative annual survey of households representing the US non-institutionalised civilian population.[Bhat…
-1024x576.jpg)
Prevalence of MDD in patients with chronic conditions
The analysis discussed here concludes that there exists a bidirectional relationship between depression and chronic illnesses.[Voinov et al., 2013]
Reference:
Voinov B, Richie WD, Bailey RK. Depression and chronic diseases: it is time for a synergistic mental health and p…
-1024x576.jpg)
Depression adds to the burden of chronic conditions
The WHO (World Health Organization) World Health Survey studied >240, 000 adults, aged ≥18 years, across 60 countries.[Moussavi et al., 2007] An average of 9.3–23.0% of participants with one or more chronic physical disease also had comorbid depression.[Moussavi et al., 2…
-1024x576.jpg)
The effect of comorbidities on patients’ quality of life
The various comorbidities of MDD (psychiatric and physical) adversely affect the quality of life of the patient.[IsHak et al., 2014; IsHak et al., 2018; Zhou et al., 2017] This emphasises the point that attending physicians need to be alive to the potential of the various…
Neuropsychiatric comorbidities
-1024x576.jpg)
Neuropsychiatric comorbidities
-1024x576.jpg)
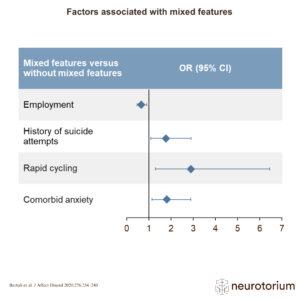
Psychiatric comorbidities of MDD
The study by Thaipisuttikul and colleagues was a cross-sectional study, conducted between October 2012 and January 2014.[Thaipisuttikul et al., 2014] In total, 190 patients with MDD, as confirmed by the Mini International Neuropsychiatric Interview (MINI), were included.[…
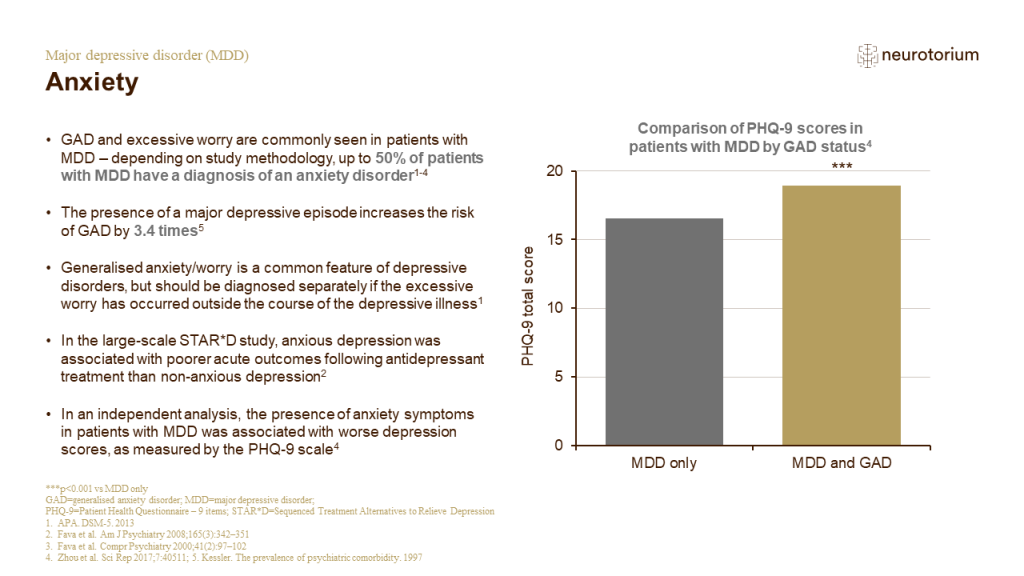
Anxiety
The Patient Health Questionnaire is a self-administered tool of 2 (PHQ-2) or 9 (PHQ-9) items.[Kroenke et al., 2001; Spitzer et al., 1999] The PHQ-9 establishes the clinical diagnosis of depression and can additionally be used to track the severity of symptoms over time.[K…
-1024x576.jpg)
Obsessive–compulsive disorder (OCD)
Obsessive-compulsive disorder (OCD) is associated with reduced quality of life, and functional impairments.[APA, 2013, pg. 240] It is defined as:[APA, 2013, pg. 237] obsession; recurrent and persistent thoughts, urges, or images, that are experienced as unwanted or intrus…
-1024x576.jpg)
Post-traumatic stress disorder (PTSD)
The essential feature of PTSD is the development of a certain set of symptoms after exposure to a traumatic event; the symptoms include fear-based re-experiencing of the traumatic event, but can also include anhedonia, and dysphoric mood states.[APA, 2013, pg. 274] Theref…
-1024x576.jpg)
Attention deficit hyperactivity disorder (ADHD)
The essential feature of ADHD is a persistent pattern of inattention and/or hyperactivity that interferes with functioning or development.[APA, 2013, pg. 61] For example, wandering off task, or difficulty sustaining focus, and excessive motor activity, or fidgeting, or ta…
-1024x576.jpg)
Schizophrenia
The essential feature of schizophrenia is the presence of hallucinations, delusions, disorganised speech or behaviour, or of negative symptoms.[APA, 2013, pg. 100] As noted on the slide, some of the diagnostic criteria for schizophrenia overlap with those for MDD, particu…
-1024x576.jpg)
Substance-use disorder
Substance-use disorders are a group of cognitive, behavioural, and physiological symptoms indicating that the individual continues to use a substance despite problems related to the use of that substance.[APA, 2013, pg. 483] Substances can include alcohol, cannabis, hallu…
-1024x576.jpg)
Neurological disorders and MDD
See Slide deck #3 of this series – ‘Neurobiology and aetiology’ to read more about the potential shared pathways underlying MDD and other neurological disorders. Disentangling the various comorbidities of MDD is a herculean challenge, because many conditions are interrela…
-1024x576.jpg)
Alzheimer’s disease (AD) and MDD
Whether or not, and to what extent, depression is a risk factor for, or a constituent part of the prodrome of, dementia, is still a contentious issue.[Cha et al., 2014; Mirza et al., 2014] One study followed >4, 300 non-demented individuals for 13.7 years, and tracked the…


-1024x576.jpg)
-1024x576.jpg)
-1024x576.jpg)
-1024x576.jpg)
-1024x576.jpg)