Slide Decks on Alzheimer’s Disease
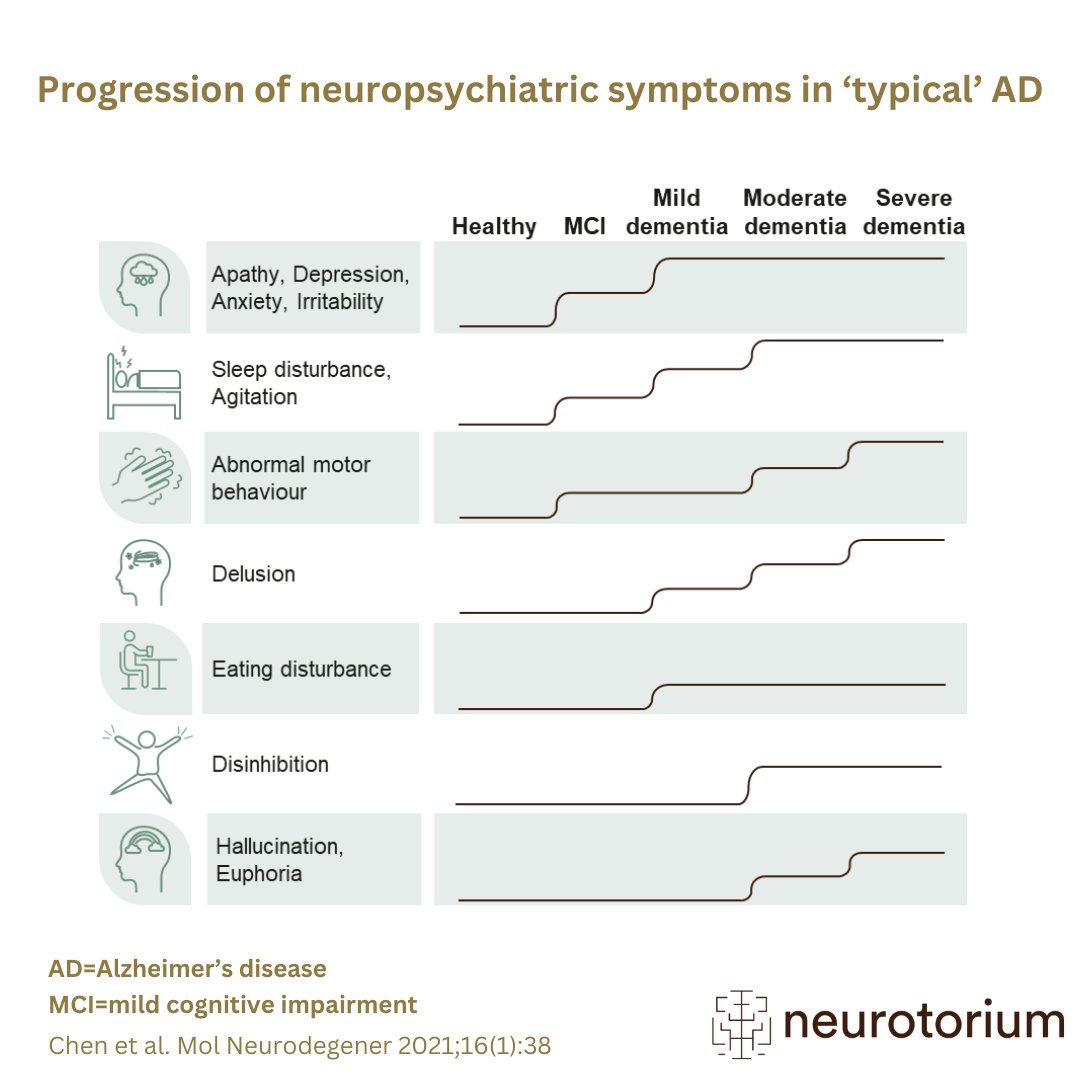
Alzheimer’s disease (AD) is a neurodegenerative disease that causes gradual cognitive decline and dementia. AD symptoms can be divided into three categories – cognitive, functional, and neuropsychiatric. Some neuropsychiatric symptoms (NPS) are key clinical manifestations of AD, with evidence that the prevalence of NPS increases with the severity of cognitive impairment. Particularly, symptoms of agitation, delusion, and irritability have been associated with worse cognitive performance.
Get an introduction to what is currently known about AD by going through our slide decks. Our slide deck is free to download and use in your presentations.
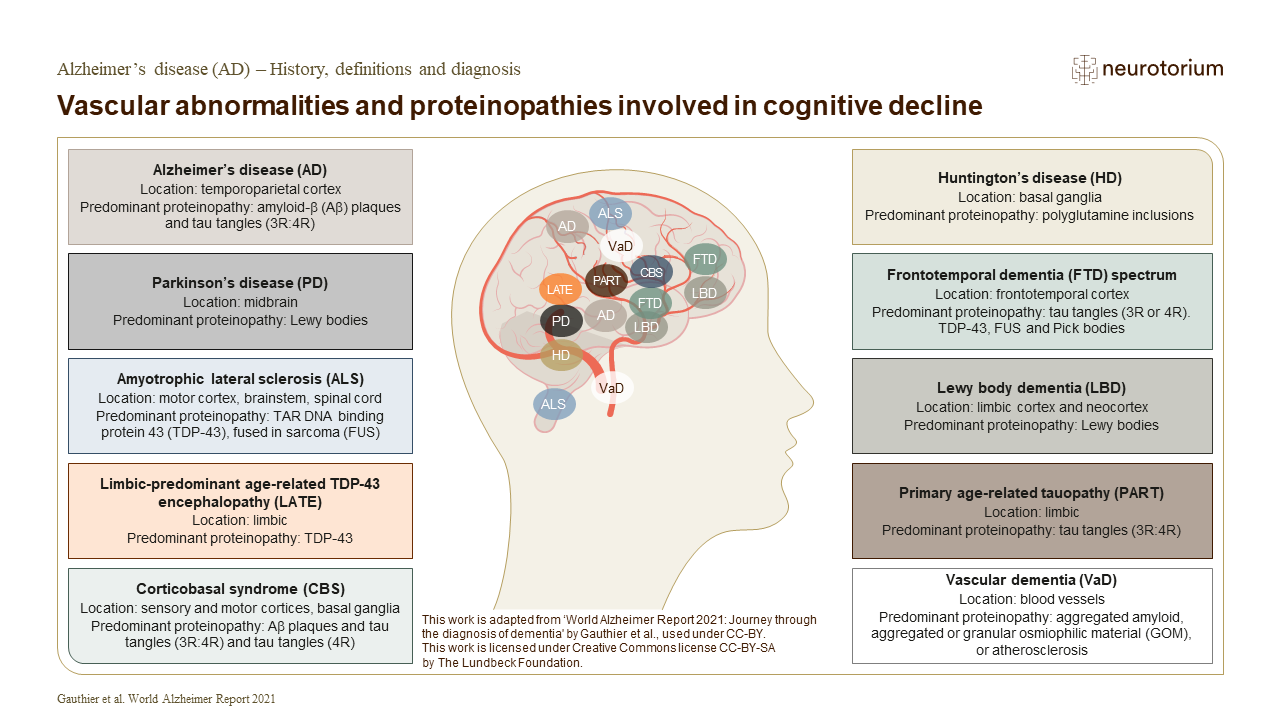
Definitions and Diagnosis
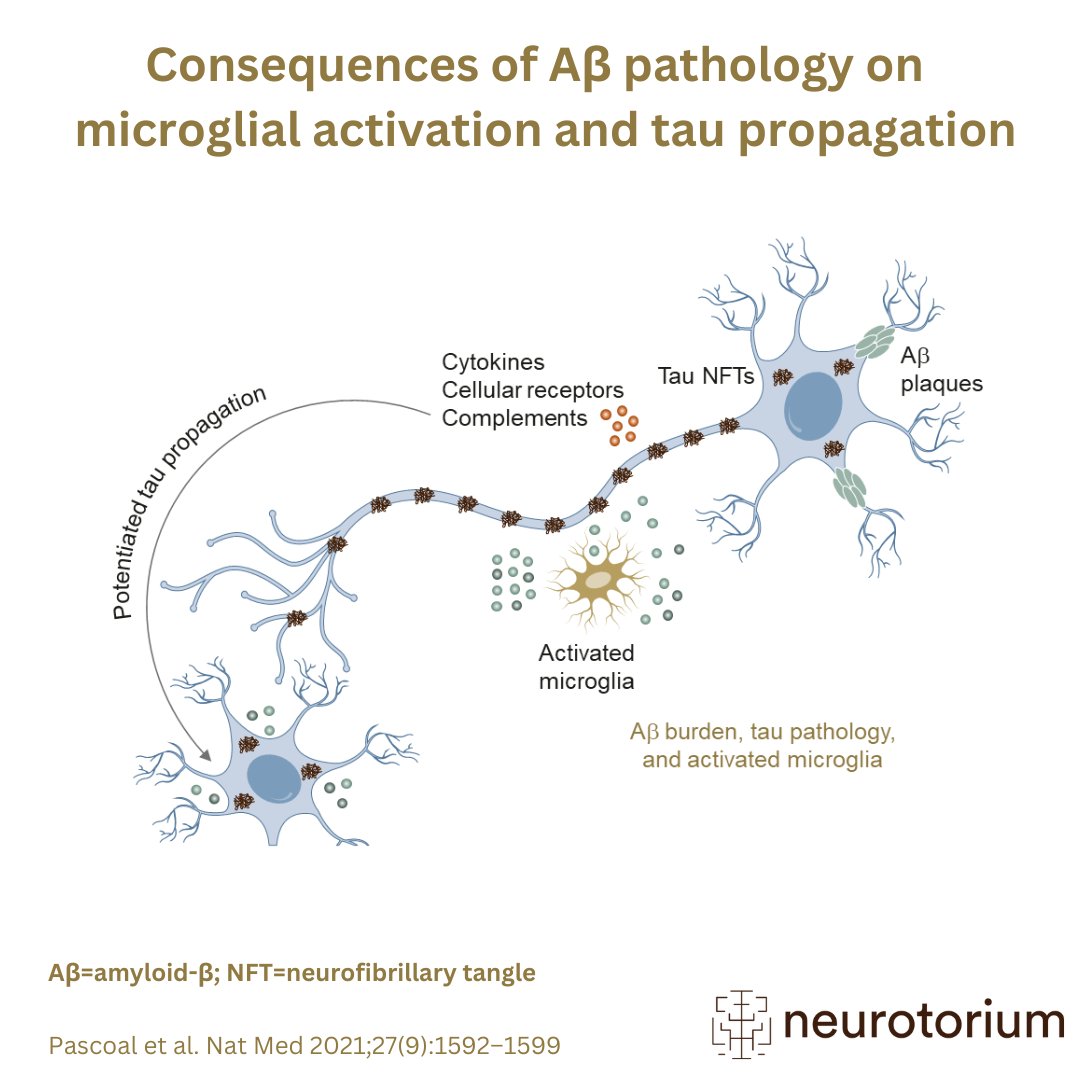
Alzheimer’s disease (AD) refers to the abnormal presence of Aβ and tau proteins, which define AD among many other neurodegenerative diseases. Go to the slide deck.
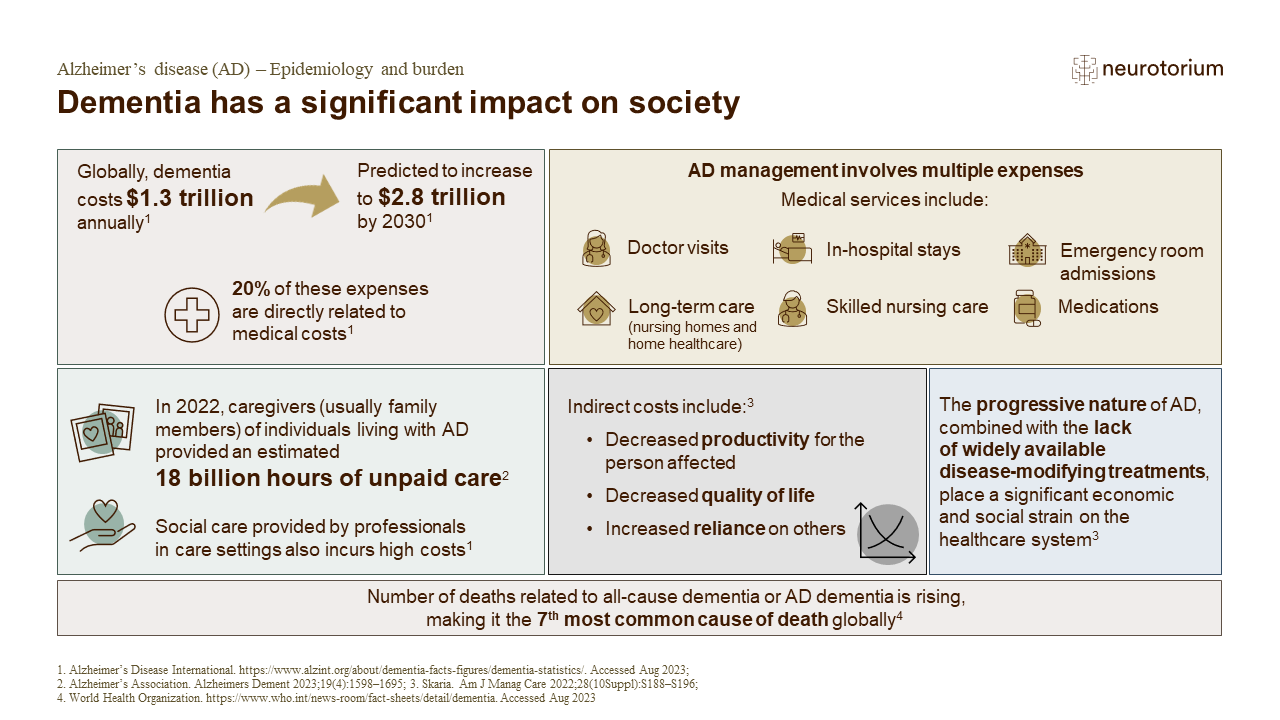
Epidemiology and Burden
This slide deck discusses the epidemiology and burden of AD and highlights topics as prevalence of dementia, burden of AD and the assessment scales for the quality of life and resource utilization in dementia. Go to the slide deck.
Neurobiology and Aetiology
This slide deck discusses neurobiology and aetiology for AD and highlights topics as risk factors, pathopsysiological hypotheses, and the development and importance of biomarkers. Go to the slide deck.
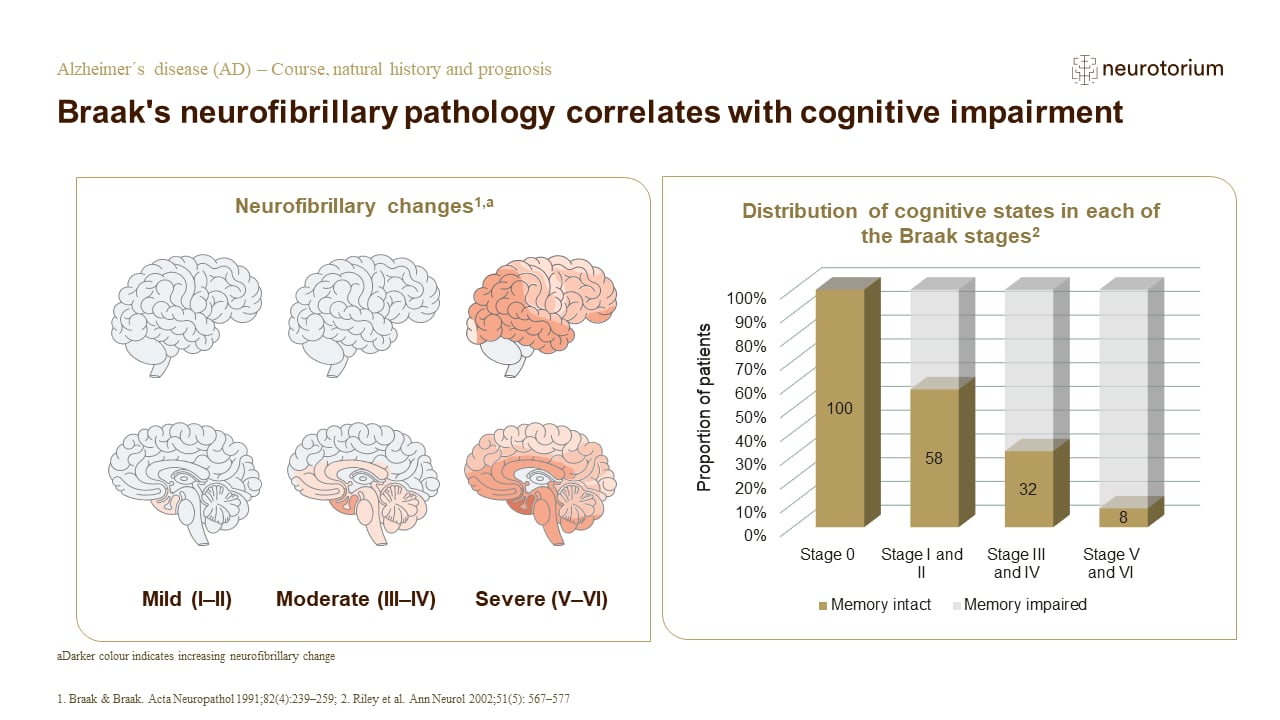
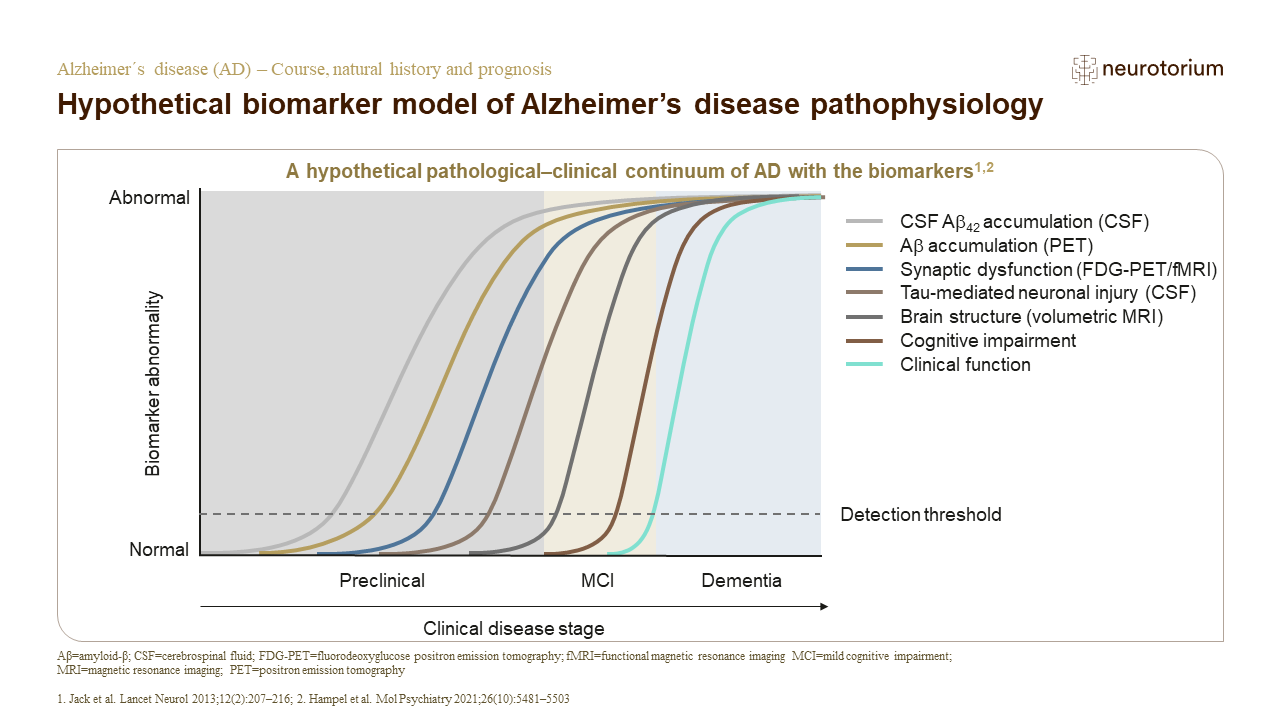
Course, Natural History and Prognosis
This slide deck discusses in detail the course, natural history and prognosis of AD, with illustrations. Go to the slide deck.
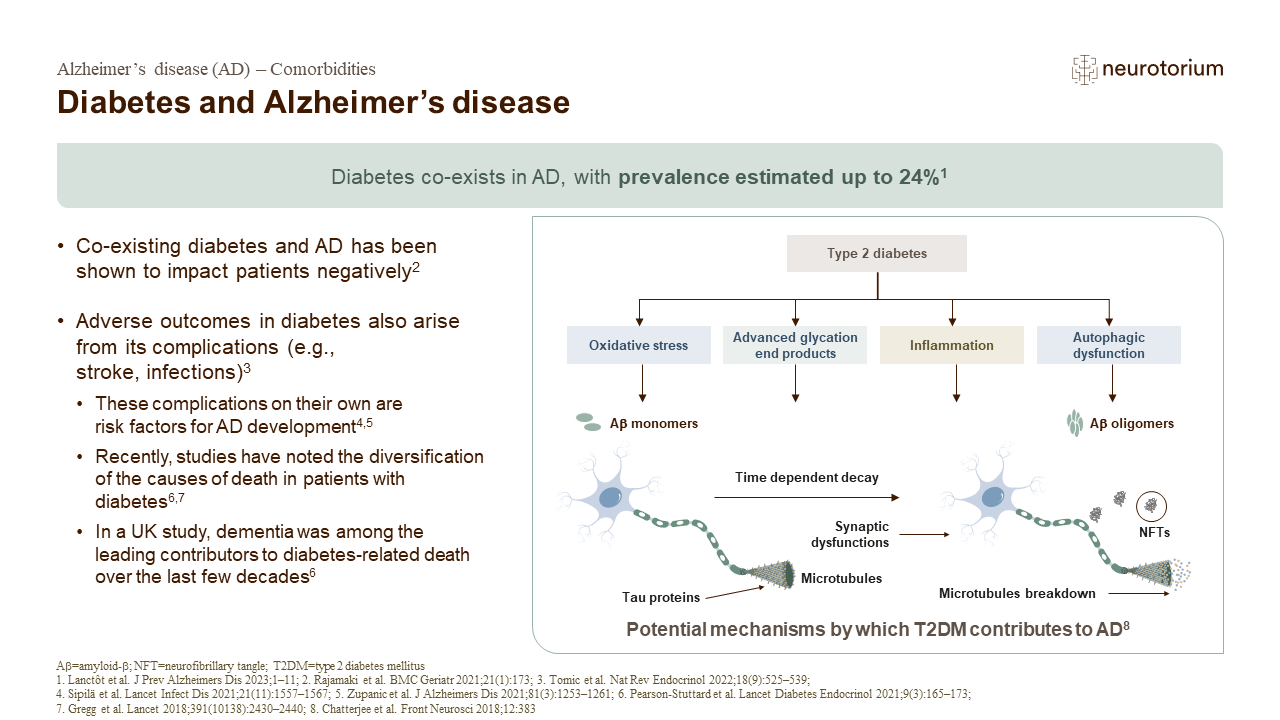
Comorbidities
This slide deck describes current knowledge on the general medical and psychiatric comorbidities of AD. Go to the slide deck.
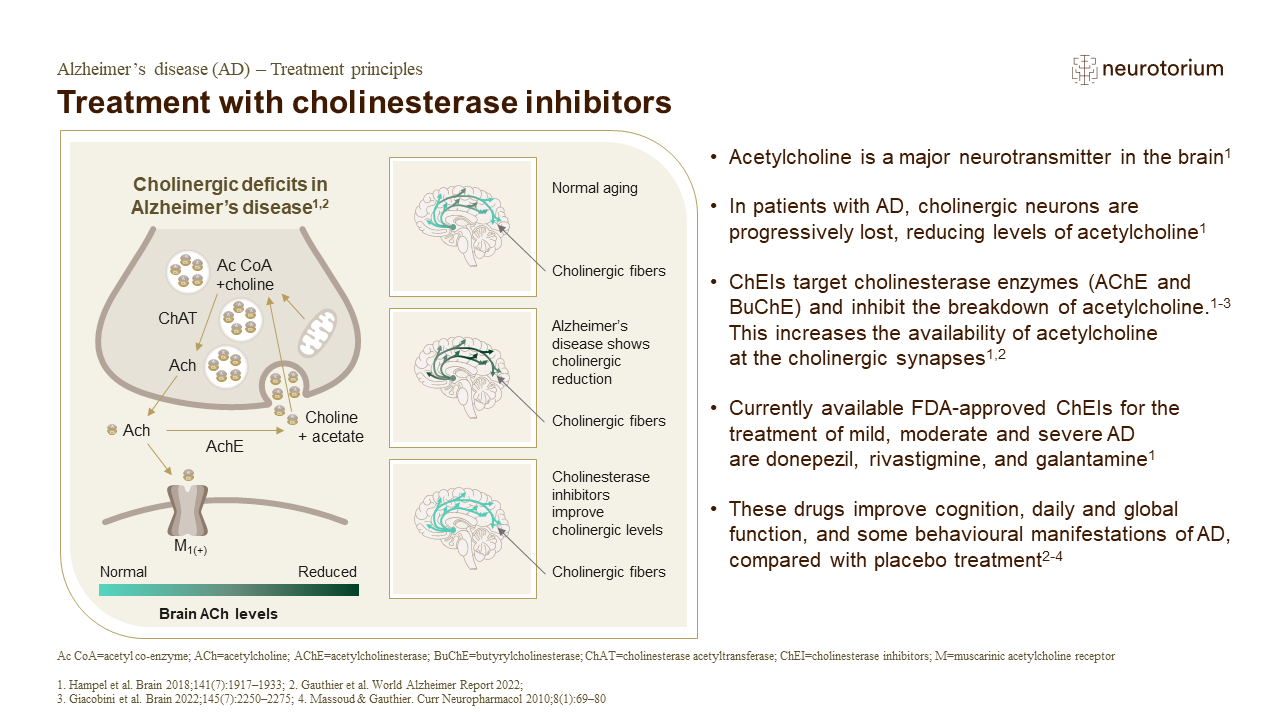
Treatment Principles
In this slide deck you will find basic concepts and definitions related to approaches such as disease-stage-specific treatment and psychosocial therapies. Go to the slide deck.
Articles on Alzheimer’s Disease
Considerable advancements in AD research have been made over the years, working towards a reality of early identification with in-vivo biomarkers and multimodal treatment of patients with AD. Several disease-modifying therapies, such as agents targeting amyloid accumulation, tau pathology, and others, are being investigated.
Watch The Videos on Alzheimer’s Disease
Access our series of videos, where we complement recent articles by explaining complex topics, breaking down detailed figures, discussing current issues, and illustrating key concepts. Dive into the varying severity of cognitive impairment in individuals living with Alzheimer’s Disease (AD) and the importance of early diagnosis for effective care, among other crucial topics.

Alzheimer’s Disease Biomarkers
In this video Joseph Therriault, PhD discusses the AD biomarkers and their use in clinical and research settings and explore future research areas for wider clinical practice use.

Alzheimer’s Disease is not synonymous with dementia
In this video, Professor Dr. Serge Gauthier explains what dementia is and what differentiates Alzheimer’s disease from other types of dementias.
Download Illustrations & Figures on Alzheimer’s Disease
Download and utilize images illustrating pertinent aspects of Alzheimer’s disease. Selected images provide insights into high-performing CSF and plasma biomarkers summarizing Alzheimer’s disease diagnosis, brain metabolism PET imaging in Alzheimer’s disease, and Amyloid-PET imaging in Alzheimer’s disease.
3D Brain Atlas
Studies indicate that biological changes in the brain begin approximately two decades before the clinical onset of AD symptoms[1]
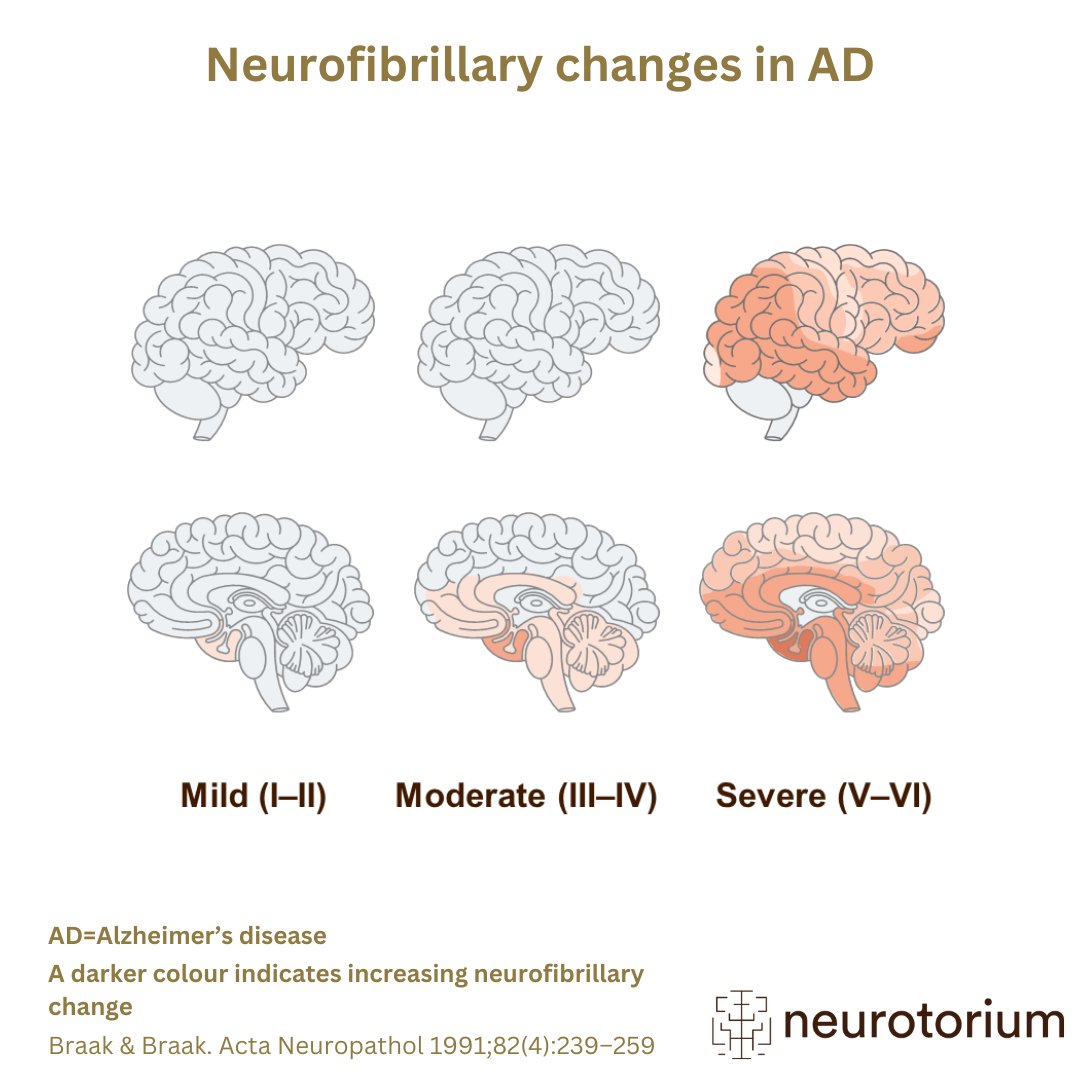
- The staging method developed by Braak and Braak suggests that the neurofibrillary pathology of AD progresses in a relatively predictable sequence across the medial temporal lobe structures, subcortical nuclei, and neocortical areas of the brain in seven stages, with the final stage representing the presence of cortical neurofibrillary changes.
- In vivo neuroimaging data from neuropathological studies show a spatiotemporal development of Aß deposits in the brain, which originates in the cerebral regions and spreads from the neocortex, to the allocortex, to the brainstem, finally reaching the cerebellum.[2,3]