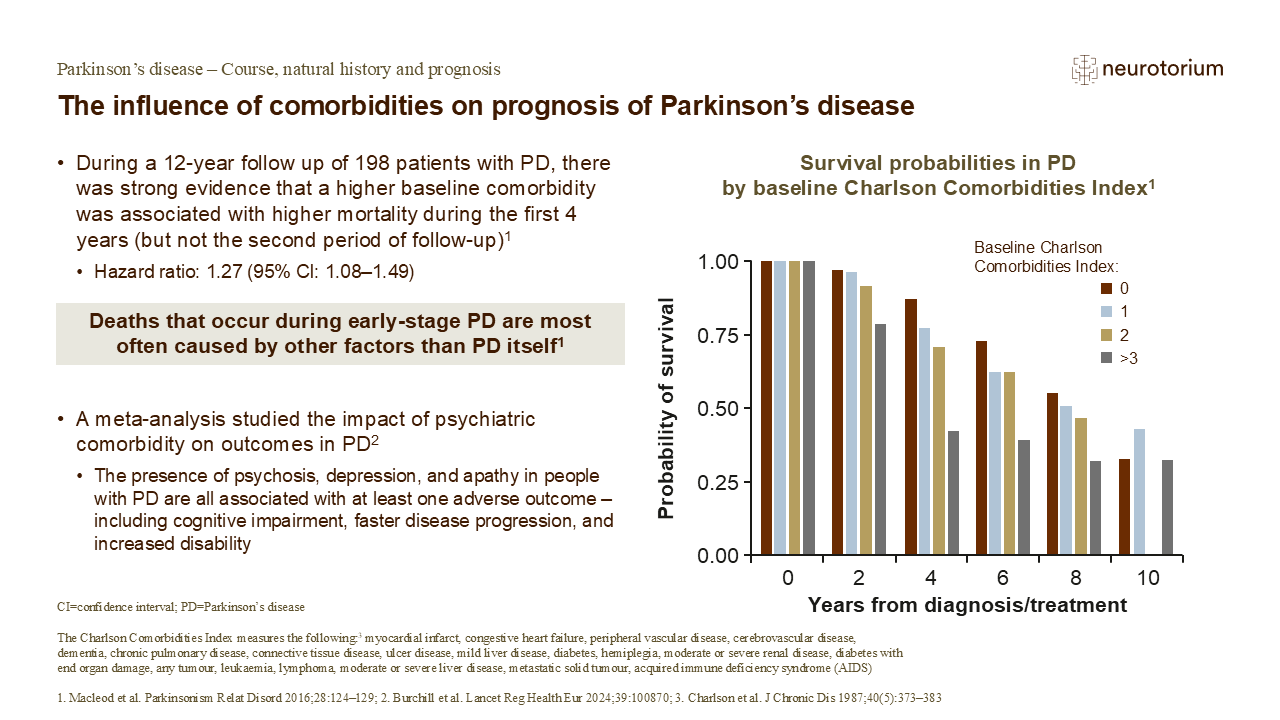
PD occurs predominantly in elderly people, who commonly have co-morbidities.1,2,4 A study that followed patients with PD over a 12-year period, concluded that having a higher level of comorbidity during the earlier stages of PD (0–4 years from diagnosis/recruitment) increased the likelihood of early death.1 Beyond 4 years, however, the amount of comorbidity in the population appeared to make little difference.1 Deaths that occur during early-stage PD are most often caused by other factors (e.g., cardiovascular disease) rather than PD itself, since PD symptoms during this period tend to be mild, easily-controlled, and unlikely to have severe adverse effects on health.1
The study also recommended the Charlson Comorbidity Index (CCI)3 as the most appropriate tool for measuring comorbidity in patients with PD; it is quicker to use and produces more consistent results than other currently available assessment methods.1