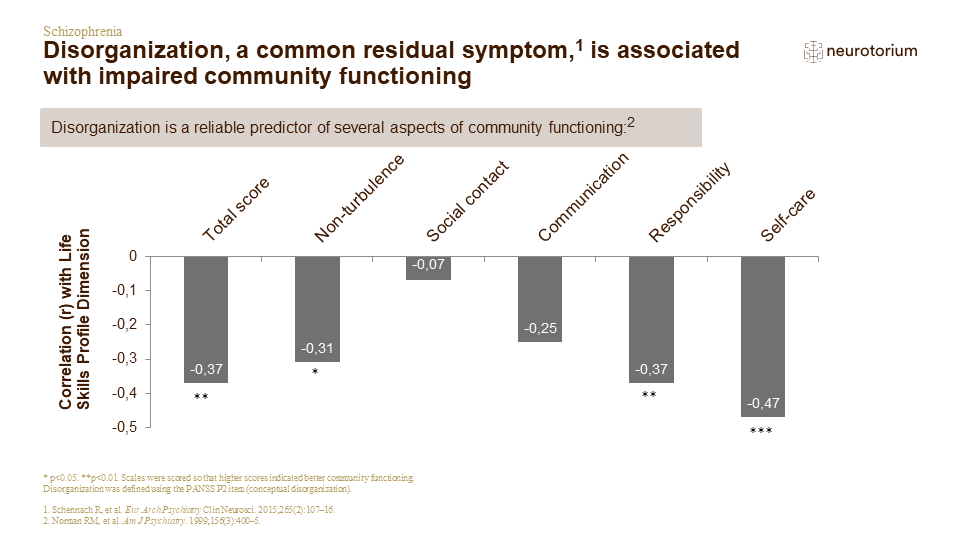
Key message: Conceptual disorganization is a common residual symptom in patients with schizophrenia, and is a reliable predictor of several aspects of community functioning, as measured by the Life Skills Profile (which was specifically designed to assess constructs of relevance to survival and adaptation in the community).
Background[Schennach R, et al., 2015]
- Conceptual disorganization is a common residual symptom in patients with schizophrenia.[Schennach R, et al., 2015]
- Conceptual disorganization occurred in 42% of patients with remission, and was the second most common residual symptom after blunted affect (which occurred in 49% of patients).[Schennach R, et al., 2015]
Background[Norman RM et al, 1999]
- Neurocognitive and symptom data (collected as part of an earlier study) were used to predict the community functioning of 50 patients (aged 17–60) with schizophrenia. Using the Life Skills Profile, staff of a community mental health program assessed community functioning while blind to the earlier symptom ratings and neurocognitive performance.[Norman RM et al, 1999]
- The Life Skills Profile was designed specifically to assess constructs of relevance to survival and adaptation in the community.
- The 39 items of the scale measure five key dimensions: self-care (grooming, hygiene, budgeting, food preparation, etc.); nonturbulence (degree of offensiveness, violence, intrusiveness, anger control, etc.); social contact (friendships, interpersonal interests and activities, etc.); communication (conversational skills, inappropriate gesturing, etc.); and responsibility (cooperativeness, responsibility regarding personal property and medication, etc.).[Norman RM et al, 1999]
- Disorganization symptoms are more strongly related than formal cognitive test scores to community functioning.[Norman RM et al, 1999]
References:
Schennach R, et al. Eur Arch Psychiatry Clin Neurosci. 2015; 265 (2): 107–16.
Norman RM, et al. Am J Psychiatry. 1999; 156 (3): 400–5.