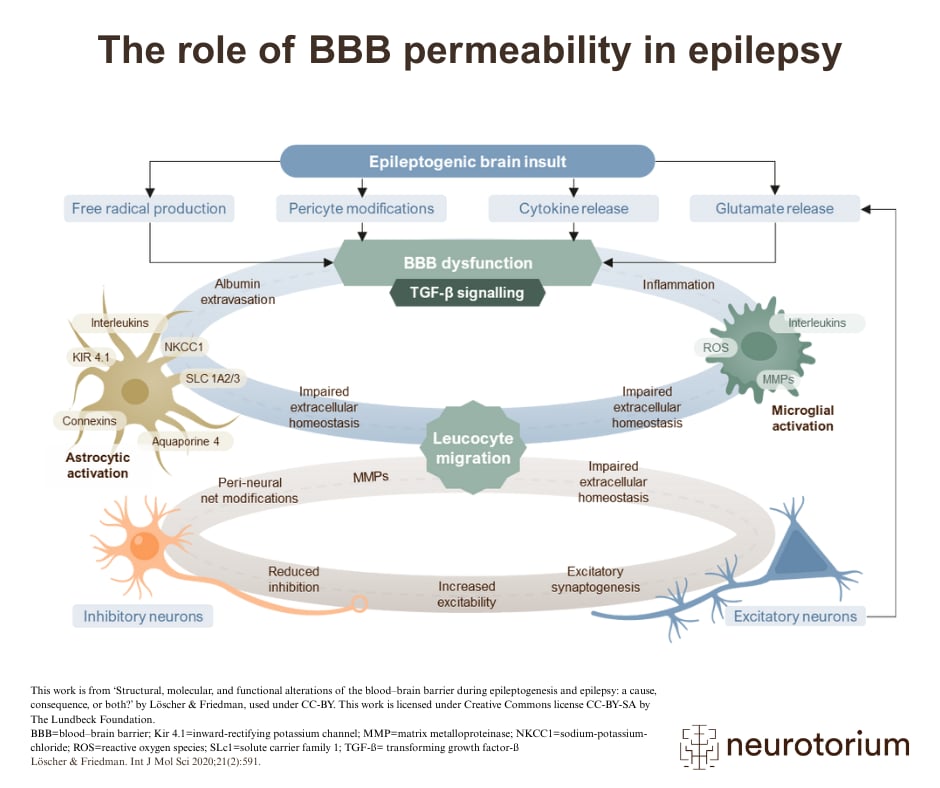
Blood–brain barrier (BBB) breakdown in epilepsy drives seizure susceptibility in a positive feedback loop, and is seen by some as a biomarker of epileptogenesis.1,2 . Several mechanisms appear to drive changes to the BBB, because there are rapid (within 30 minutes) increases in permeability together with a more lasting effect over hours.1 A direct result of a seizure is increased levels of glutamate, which increases the activity of matrix metalloproteinases that degrade the extracellular matrix surrounding capillaries and the integrity of the endothelium. Seizures also contribute to pericyte dysfunction, as well as activation of glia, release of reactive oxygen species and cytokines, and extravasation of immune cells.
Although complex, and not completely understood, BBB damage and permeability can be seen as both a consequence and a trigger of seizures.1,2
BBB=blood–brain barrier; Kir 4.1=inward-rectifying potassium channel; MMP=matrix metalloproteinase; NKCC1=sodium-potassium-chloride; ROS=reactive oxygen species; SLc1=solute carrier family 1; TGF-ß= transforming growth factor-ß