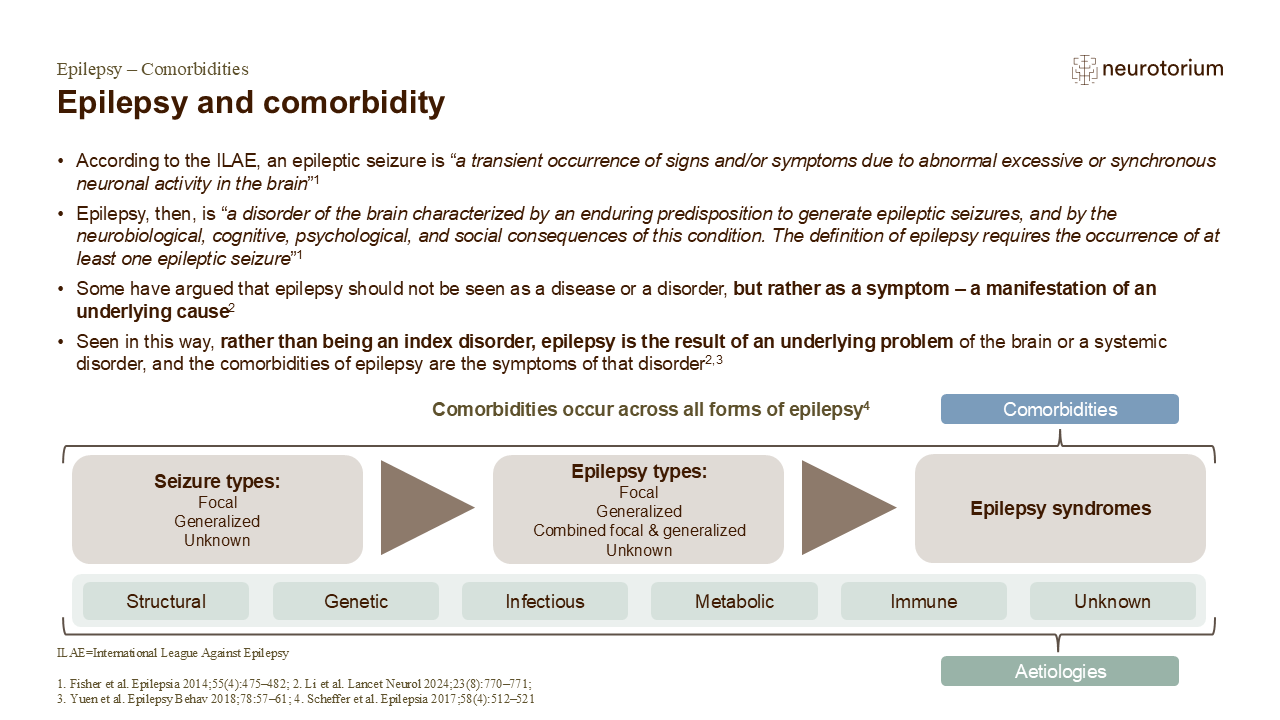
The aetiology of epilepsy has important implications for treatment.4 Multiple aetiologies may apply to an individual patient; they are not hierarchical, and the importance ascribed to a patient’s aetiological group may depend on their specific circumstances.4 Worldwide, epilepsy most commonly occurs as a direct result of an infection in which seizures are a core symptom of the disorder; it is important to note that ‘infectious aetiology’ refers to a person with epilepsy, not to a person with seizures occurring in the context of an acute infection such as meningitis.4
Many epilepsies are associated with comorbidities such as learning, psychological or behavioural problems, ranging in type and severity from subtle learning difficulties to intellectual disability, psychiatric disorders or psychosocial concerns.4 In more severe epilepsies, patients may suffer from a complex range of comorbidities including cerebral palsy, movement disorders, sleep and gastrointestinal disorders.4 Like aetiology, the presence of comorbidities should be considered at every stage of epilepsy treatment, to ensure appropriate management.4
References: