Index for
slide deck
Introduction

Major depressive disorder (MDD) - Comorbidity

Defining comorbidity
Although attempts have been made to define comorbidity, including the seminal work of the 1970s, it is a term that is used with different meaning across the scientific literature.1,3 Moreover, beyond comorbidity, multimorbidity is used to discuss the presence of several m…

Neuropsychiatric comorbidities in patients with depression
Neuropsychiatric comorbidities occur in approximately 70% of people with MDD – this prevalence generally increases with depression severity, ranging from 64% comorbidity prevalence rate in people with mild depression to a 78% prevalence rate in people with severe MDD.1,2
…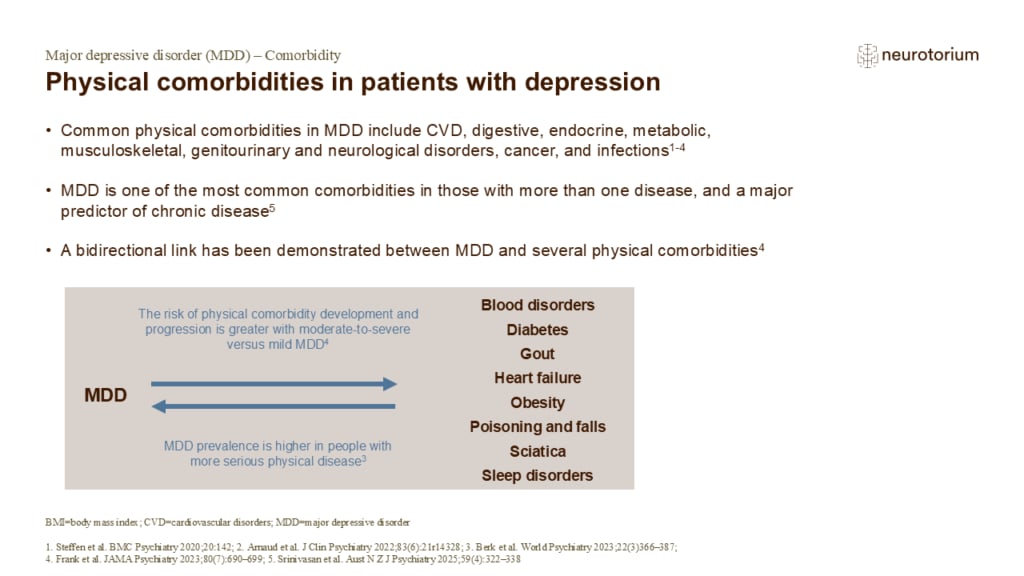
Physical comorbidities in patients with depression
Common physical comorbidities in MDD include cardiovascular disease (e.g., coronary heart disease, hypertension, myocardial infarction), digestive and metabolic disorders (type 2 diabetes, obesity, gastritis and duodenitis, non-infectious gastroenteritis) musculoskeletal …
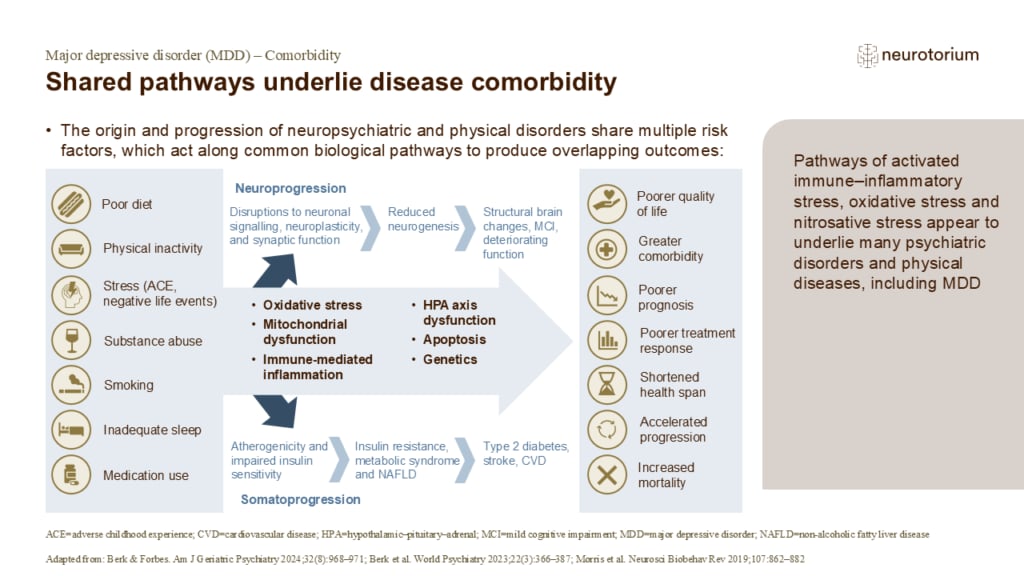
Shared pathways underly disease comorbidity
Mitochondrial function (i.e., ATP production) is impaired in people with MDD compared with controls, leading to inefficient respiration and the production of reactive oxygen species, resulting in oxidative stress.2 In addition, MDD has neuroendocrine effects, including sy…

Prevalence of chronic conditions in patients with MDD
In this study, data from the 2007 and 2009 releases of the Medical Expenditure Panel Survey (MEPS) were used.1 The MEPS is a nationally representative annual survey of households representing the US non-institutionalised civilian population.1 After inclusion/exclusion cri…
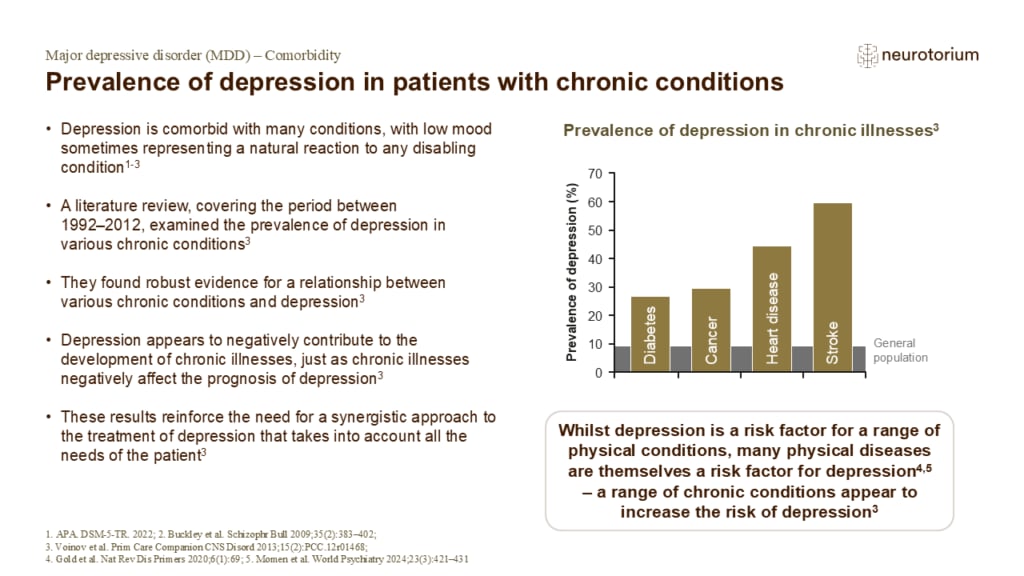
Prevalence of depression in patients with chronic conditions
The analysis discussed here concludes that there exists a bidirectional relationship between depression and chronic illnesses.3
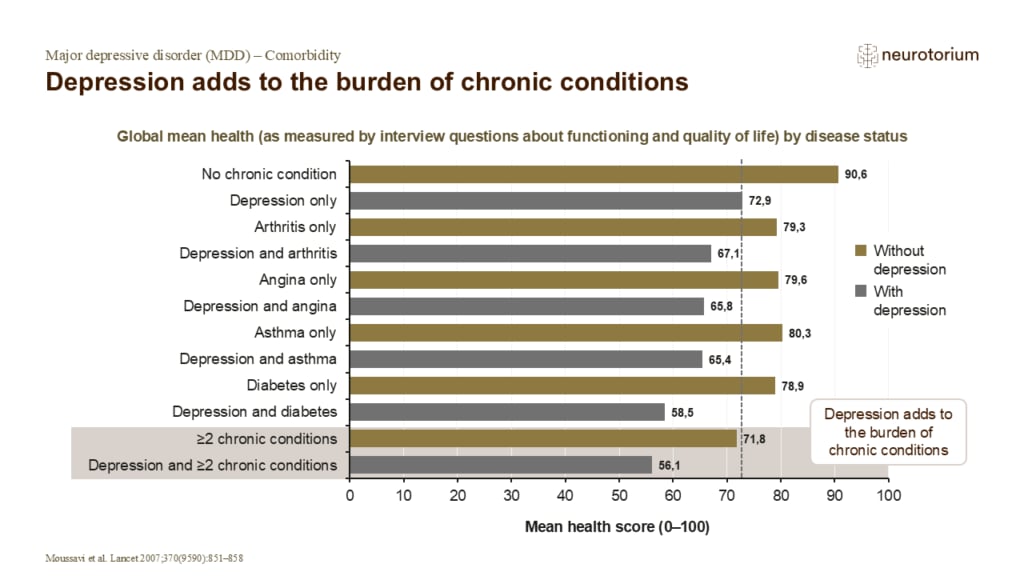
Depression adds to the burden of chronic conditions
The WHO (World Health Organization) World Health Survey studied >240,000 adults, aged ≥18 years, across 60 countries.1
An average of 9.3–23.0% of participants with one or more chronic physical disease also had comorbid depression.1 Individuals with a chronic condition wer…
The effect of comorbidities on patients’ quality of life
The various comorbidities of MDD (psychiatric and physical) adversely affect the quality of life of the patient.1-3 This emphasizes the point that attending physicians need to be alert to the potential of the various comorbidities when treating any patient with MDD.4
Trea…
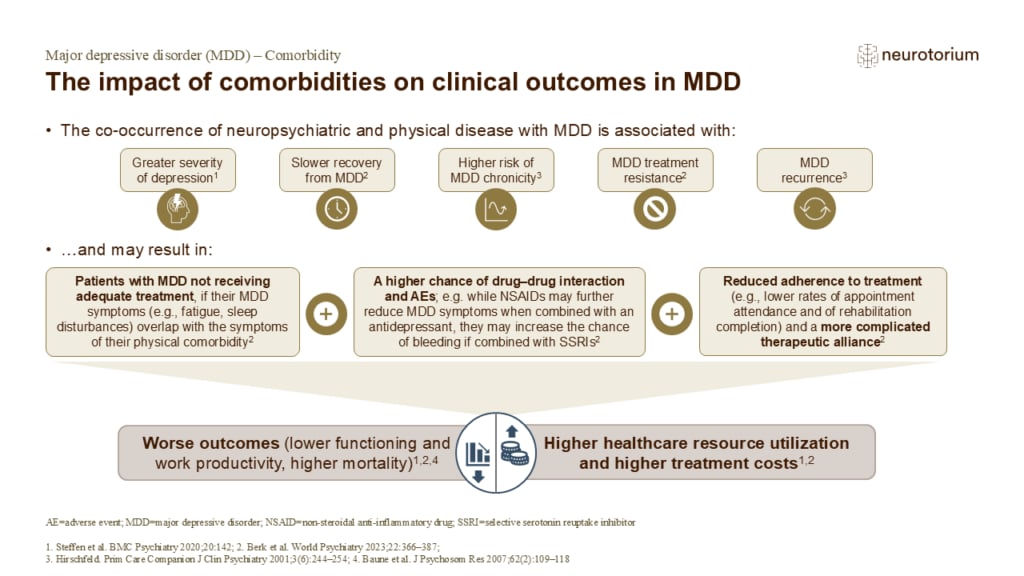
The impact of comorbidities on clinical outcomes in MDD
The presence of psychiatric and physical comorbidities adversely affects health outcomes and general functioning, and increases treatment costs and healthcare resource utilization in people with MDD.2,4 MDD comorbid with another medical disorder is also strongly associate…

Treatment application of the link between MDD and comorbidities
Data from studies suggests that reducing depressive symptoms is associated with significant improvements in many comorbid diseases, including substance abuse, CNS, and musculoskeletal disorders.1 In cardiovascular and metabolic disorders (particularly myocardial infarctio…